 Global Health Management Services has partnered with Mingle Analytics to bring you industry leading Medicare quality reporting products and services for MIPS and the Quality Payment Program.
Global Health Management Services has partnered with Mingle Analytics to bring you industry leading Medicare quality reporting products and services for MIPS and the Quality Payment Program.
Founded by nationally-recognized expert on quality reporting, CEO Dan Mingle, M.D., MIPS Solutions brings together expert Consultants and Cutting Edge Tools to guide you every step of the way to succeed with Medicare quality reporting programs.
Succeeding with MIPS and the Quality Payment Program
What is MIPS?
Medicare’s newest program, the Merit-Based Incentive Payment System (MIPS), begins January 1, 2017, and combines PQRS, Value Modifier, and Meaningful Use into a single program.
What’s at stake?
2018 is the second year of MIPS — providers and practices have the potential to lose up to 5% of their Medicare reimbursements in 2020 based on their 2018 MIPS Final Score. Since 2018 is another transition year, it’s easy to participate and avoid a penalty for most MIPS eligible clinicians.
Does MIPS apply to me?
For the first two performance years of MIPS, an Eligible Clinician (previously known as an Eligible Provider in the retired PQRS program) is defined by CMS as a Physician, Physician Assistant, Nurse Practitioner, Clinical Nurse Specialist, or Certified Registered Nurse Anesthetist.
Clinicians are exempt in 2018 if any of the following apply to them:
- Qualifying participant in an advanced APM
- First year provider in Medicare Part B PFS
- Treat ≤200 Medicare patients or have
≤$90,000 in Medicare Part B allowable charges
What am I scored on under MIPS?
In 2018, the points you receive in four weighted performance categories comprise your Final Score, which is calculated by CMS.
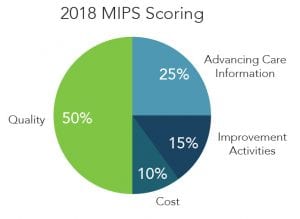
Will I need a Registry under MIPS?
Under MIPS, the Registry method is more convenient and effective than ever. CMS allows Quality, Advancing Care Information, and Improvement Activities to be submitted through a single vendor with a common deadline of March 31.
The Cost performance category is calculated by CMS based on claims data submitted throughout the year.
In addition, there are additional submission options available. Ultimately, you choose the best method for you and your practice.
Contact Us Today
Global Health Management Services and Mingle Analytics will help you avoid penalties and succeed with MIPS and the Quality Payment Program.
Phone: 1-888-610-2455 or visit: mingleanalytics.com/ghms
Avoid penalties and earn incentives under the Quality Payment Program
In 2018, it’s easy to avoid a penalty and most practices will be able to earn an incentive and potential bonus. You can trust MIPS Solutions to guide you every step of the way with a solution tailored to your needs.
Manage all components of the program in one place.
The tools help you track the status of your reporting and stay informed about your progress.
Understand the measures that are best for you and your practice.
Use our analyzers and guides to make an informed decision about measures most applicable to your organization.
Analyze and track your performance.
Review performance by practice and provider continuously, quarterly, or annually. Extend your reporting capability with data integration.
Send your data to Medicare for all programs and payment models.
- Qualified Registry for QPP (MIPS & APMs)
- Data Submission Vendor (DSV)
- ACO Reporting
How to Get Started with MIPS
- Visit mingleanalytics.com/ghms to sign up for a user account
- Log into your user account and register your organization
- Purchase MIPS Solutions to begin your engagement (don’t forget to use your exclusive coupon)
Visit mingleanalytics.com/ghms to sign up

Have questions?
Contact Global Health Management Services at 1-888-610-2455 or Mingle Analytics at 1-866-359-4458
*Global Health Management Services has partnered with Mingle Analytics to bring you exclusive discounts and unparalleled customer support with MIPS Solutions.
Ready to get started with MIPS and the Quality Payment Program?
Visit mingleanalytics.com/ghms to learn more and register for MIPS Solutions
